11.1 – Introduction to Major Minerals
Learning Objective
- Describe the role, intake recommendations and sources of major minerals

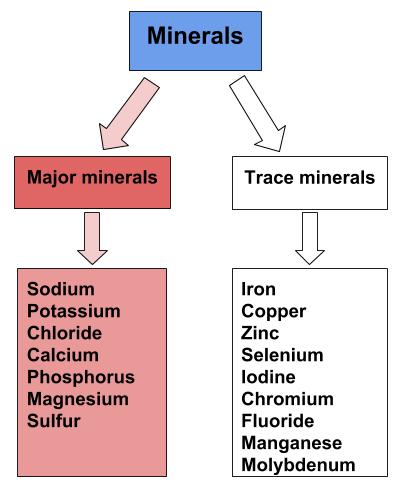
Major minerals are classified as minerals that are required in the diet each day in amounts larger than 100 milligrams. These include sodium, potassium, chloride, calcium, phosphorus, magnesium, and sulfur. These major minerals can be found in various foods. For example, in Guam, the major mineral, calcium, is consumed in the diet not only through dairy, a common source of calcium but also through the mixed dishes, desserts, and vegetables that they consume. Consuming a varied diet significantly improves an individual’s ability to meet their nutrient needs. 1
1 Pobocik RS, Trager A, Monson LM. Dietary Patterns and Food Choices of a Population Sample of Adults on Guam. Asia Pacific Journal of Clinical Nutrition. 2008; 17(1), 94-100. http://apjcn.nhri.org.tw/server/APJCN/17/1/94.pdf. Accessed June 30, 2019.
Bioavailability
Minerals are not as efficiently absorbed as most vitamins and so the bioavailability of minerals can be very low. Plant-based foods often contain factors, such as oxalate and phytate, that bind to minerals and inhibit(interfere with) their absorption. In general, minerals are better absorbed from animal-based foods. In most cases, if the dietary intake of a particular mineral is increased, absorption will decrease. Some minerals influence the absorption of others. For instance, excess zinc in the diet can impair iron and copper absorption. Conversely, certain vitamins enhance mineral absorption. For example, vitamin C boosts iron absorption, and vitamin D boosts calcium and magnesium absorption. As is the case with vitamins, certain gastrointestinal disorders and diseases, such as Crohn’s disease and kidney disease, as well as the aging process, impair mineral absorption, putting people with malabsorption conditions and the elderly at higher risk for mineral deficiencies.
| Micronutrient | Sources | Recommended Intake for Adults | Functions | Deficiency Diseases and Symptoms | Groups at Risk of Deficiency | Toxicity | U.L. |
|---|---|---|---|---|---|---|---|
| Calcium | Yogurt, cheese, sardines, milk, orange juice, turnip | 1,000 mg/day | Component of mineralized bone, provides structure and microarchitecture | Increased risk of osteoporosis | Postmenopausal women, those who are lactose intolerant, or vegan | Kidney stones | 2,500 mg |
| Phosphorus | Salmon, yogurt, turkey, chicken, beef, lentils | 700 mg/day | The structural component of bones, cell membrane, DNA and RNA, and ATP | Bone loss, weak bones | Older adults, alcoholics | None | 3,000 mg |
| Magnesium | Whole grains and legumes, almonds, cashews, hazelnuts, beets, collards, and kelp | 420 mg/day | Component of mineralized bone, ATP synthesis and utilization, carbohydrate, lipid, protein, RNA, and DNA synthesis | Tremor, muscle spasms, loss of appetite, nausea | Alcoholics, individuals with kidney and gastrointestinal disease | Nausea, vomiting, low blood pressure | 350 mg/day |
| Sulfur | Protein foods | None specified | Structure of some vitamins and amino acids, acid-base balance | None when protein needs are met | None | None | N D |
| Sodium | Processed foods, table salt, pork, chicken | < 2,300 mg/day; ideally 1,500 mg/day | Major positive extracellular ion, nerve transmission, muscle contraction, fluid balance | Muscle cramps | People consuming too much water, excessive sweating, those with vomiting or diarrhea | High blood pressure | 2,300 mg/day |
| Potassium | Fruits, vegetables, legumes, whole grains, milk | 4700 mg/day | Major positive intracellular ion, nerve transmission, muscle contraction, fluid balance | Irregular heartbeat, muscle cramps | People consuming diets high in processed meats, those with vomiting or diarrhea | Abnormal heartbeat | N D |
| Chloride | Table salt, processed foods | < 3600 mg/day; ideally 2300 mg/day | Major negative extracellular ion, fluid balance | Unlikely | None | None | 3,600 mg/day |
Key Takeaways
- See the Table above for a summary of the major minerals.
Contributors
The University of Hawai’i at Mānoa Food Science and Human Nutrition Program: Allison Calabrese, Cheryl Gibby, Billy Meinke, Marie Kainoa Fialkowski Revilla, and Alan Titchenal

